Unmasking the Hidden Trauma: The Link Between Concussion, Domestic Violence, and Mental Health
- Secretary Perth
- Oct 12, 2023
- 6 min read
Updated: Oct 13, 2023

In the quiet corners of a bustling world, a silent crisis often goes unnoticed - one that affects millions of women and leaves a lasting impact on their lives. It's a crisis at the intersection of traumatic brain injury, domestic violence, and mental health. Dr. Sarah Hellewell, a Senior Research Fellow in Neurotrauma at Curtin University and the Perron Institute for Neurological and Translational Science, is shedding light on this under-recognized issue.
Understanding Concussion and Its Prevalence:
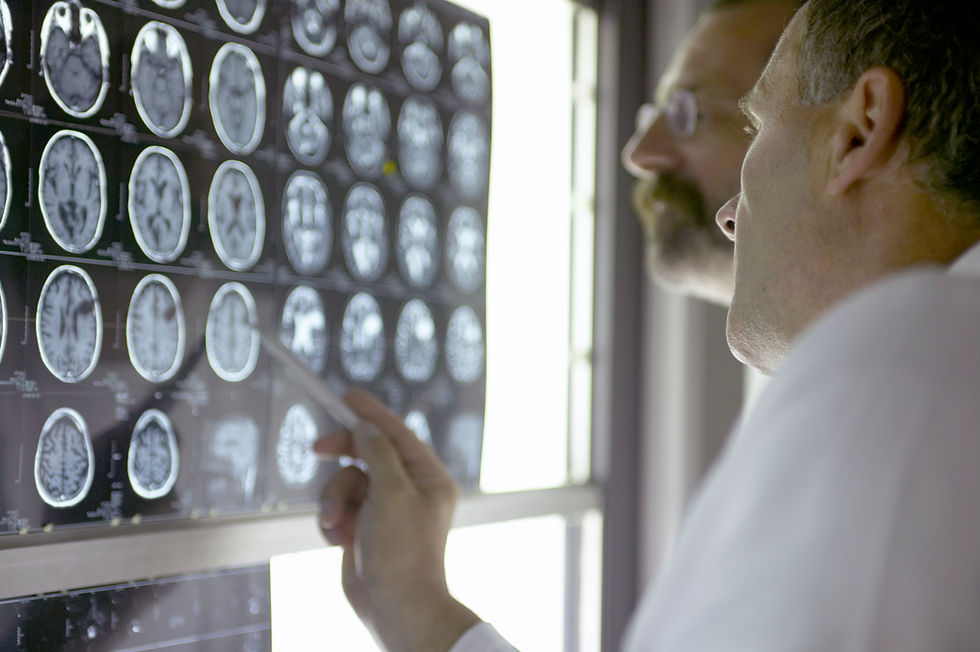
Concussion, the most common form of traumatic brain injury, is often associated with sports, military service, and accidents. Yet, it's essential to acknowledge that anyone can experience a concussion, and the statistics are staggering - in Australia, there is estimated to be over 170,000 cases of concussion per year.
However, the startling truth is that up to half of those who suffer concussions recover poorly and face persistent symptoms. The likelihood of poor recovery increases with the number of concussions experienced, leading to recognized links between repeated brain injuries mental health issues and long-term brain degeneration.
The Hidden Dangers for Survivors of Domestic Violence:
Dr. Sarah Hellewell's groundbreaking work has illuminated a crucial, yet under-discussed aspect of this issue - the heightened risk that survivors of domestic violence face when it comes to concussions. In Australia, it is estimated that 40% of hospital admissions related to family violence have documented cases of head injuries. Often, their injuries go unnoticed, and symptoms are misdiagnosed. As a result, women trapped in abusive relationships may experience repeated concussions, unknowingly exposing themselves to long-term consequences.
Recognizing the complexities surrounding the identification of injuries resulting from domestic violence (DV) is essential. for instance, victims often face barriers to seeking immediate medical care due to the high-risk nature of their situations, fear of their abusers or a lack of awareness and education on the part of victims regarding the potential health consequences of such injuries, which can lead to a lack of urgency in seeking medical treatment. These circumstances can result in victims returning to their partners repeatedly, heightening the risk of sustained exposure to injuries that, if left untreated for extended periods, may lead to traumatic brain injuries (TBIs).
Additionally, there are significant limitations in the education around the screening process for concussion in DV victims, not only in hospital settings but also in support services and police stations. It is crucial to address these gaps by providing education and training to professionals within the criminal justice and healthcare sectors on how to effectively screen for domestic violence and potential head injuries resulting from such violence.
“women trapped in abusive relationships may experience repeated concussions, unknowingly exposing themselves to long-term consequences.”
Long-Term Implications:
The long-term implications of concussions, especially for survivors of domestic violence, are both profound and alarming. Research suggests that repeated concussions can lead to serious brain degeneration, resulting in cognitive and neuropsychological outcomes that significantly impact a person's life.
Moreover, there's a growing body of evidence linking concussions to mental health disorders. The repercussions of untreated or unrecognized concussions can extend far beyond the initial injury, manifesting as depression, anxiety, post-traumatic stress disorder (PTSD), and other mental health challenges.
What can we do?
So, what can be done to address this hidden crisis? Dr. Sarah Hellewell's research underscores the importance of early recognition and intervention. Implementing screening tools such as Ohio State University TBI Identification Method (for TBI) and the Partner Violence Screen Questionnaire (for DV) for both healthcare providers and domestic violence survivors can make a significant difference. These tools can help identify concussions, even in cases where the symptoms are subtle or masked by other injuries.
Dr. Sarah Hellewell's work has revealed the intricate relationship between concussion, domestic violence, and mental health, emphasizing the need for increased awareness and action. It's crucial to recognize that concussions are not just sports injuries; they can affect anyone, with long-term implications that extend far beyond the initial injury.
Raising awareness about concussions in the context of domestic violence (DV) is essential to ensure that victims receive proper medical attention and support. Individuals and organizations like Zonta can take various strategies to achieve this goal:
1. Education and Training:
Raise awareness among friends, family, and community members about the link between DV and concussion. Encourage open discussions to help victims recognize the signs and seek help.
Offer training sessions and workshops for members to educate them about the connection between DV and concussion. Collaborate with experts to provide up-to-date information.
2. Outreach and Awareness Campaigns:
Use social media, personal blogs, or community events to share information and stories related to DV-related concussions. Engage in conversations to debunk myths and misconceptions.
Launch awareness campaigns that target a wider audience. Develop informative materials, such as brochures, posters, or online resources, and distribute them through various channels.
3. Collaboration with Healthcare Providers:
Encourage victims to seek medical attention and share information about DV-related concussions with healthcare providers. Advocate for better training for healthcare professionals.
Collaborate with local healthcare institutions to develop protocols for screening and identifying concussion in DV cases. Provide resources for healthcare professionals to recognize the signs.
4. Support for Victims:
Offer emotional support to DV survivors and encourage them to prioritize their health. Help them access resources for medical evaluation and counselling.
Establish partnerships with local DV support organizations and shelters to provide information on concussions. Fund programs that offer medical assessments and counselling to survivors.
5. Legal and Policy Advocacy:
Advocate for stronger legal protections and policies that address DV-related concussions. Join or support organizations working on DV policy reform.
Lobby for legislative changes that recognize the specific risks and consequences of DV-related concussions. Collaborate with other advocacy groups to amplify the message.
6. Research and Data Collection:
Encourage survivors to share their experiences anonymously for research purposes. Participate in studies that examine the prevalence and impact of DV-related concussions.
Support or conduct research projects that investigate the link between DV and concussion. Use the findings to raise awareness and advocate for better support systems.
7. Trauma-Informed Approach:
Approach DV survivors with empathy and understanding. Be mindful of the potential trauma associated with concussion and avoid victim-blaming.
Promote a trauma-informed approach within the community and among members. Encourage respectful and supportive interactions with survivors.
8. Collaboration with Other Organizations:
Connect with local DV support groups, women's organizations, and healthcare professionals to form a united front in raising awareness about DV-related concussions.
Forge partnerships with other like-minded organizations to pool resources and amplify advocacy efforts. Collaborative initiatives often have a more significant impact.
By taking these steps and supporting survivors of domestic violence, we can take significant steps toward unmasking the hidden trauma and helping those who need it most. Together, we can pave the way for better understanding, care, and support for survivors on their journey to recovery.
Help support our projects by making a tax-deductable donation to the Perth Foundation for Women: https://lnkd.in/gtYbu-pi
References:
Thomas E, Fitzgerald M, Cowen G. Post-concussion states: How do we improve our patients’ outcomes? An Australian perspective. Journal of Concussion. 2020;4. doi:10.1177/2059700220960313
Kathleen Baxter & Sarah C. Hellewell (2019) Traumatic Brain Injury within Domestic Relationships: Complications, Consequences and Contributing Factors, Journal of Aggression, Maltreatment & Trauma, 28:6, 660-676, DOI: 10.1080/10926771.2019.1602089
Stein MB, Jain S, Giacino JT, Levin H, Dikmen S, Nelson LD, Vassar MJ, Okonkwo DO, Diaz-Arrastia R, Robertson CS, Mukherjee P, McCrea M, Mac Donald CL, Yue JK, Yuh E, Sun X, Campbell-Sills L, Temkin N, Manley GT; TRACK-TBI Investigators; Adeoye O, Badjatia N, Boase K, Bodien Y, Bullock MR, Chesnut R, Corrigan JD, Crawford K, Diaz-Arrastia R, Dikmen S, Duhaime AC, Ellenbogen R, Feeser VR, Ferguson A, Foreman B, Gardner R, Gaudette E, Giacino JT, Gonzalez L, Gopinath S, Gullapalli R, Hemphill JC, Hotz G, Jain S, Korley F, Kramer J, Kreitzer N, Levin H, Lindsell C, Machamer J, Madden C, Martin A, McAllister T, McCrea M, Merchant R, Mukherjee P, Nelson LD, Noel F, Okonkwo DO, Palacios E, Perl D, Puccio A, Rabinowitz M, Robertson CS, Rosand J, Sander A, Satris G, Schnyer D, Seabury S, Sherer M, Stein MB, Taylor S, Toga A, Temkin N, Valadka A, Vassar MJ, Vespa P, Wang K, Yue JK, Yuh E, Zafonte R. Risk of Posttraumatic Stress Disorder and Major Depression in Civilian Patients After Mild Traumatic Brain Injury: A TRACK-TBI Study. JAMA Psychiatry. 2019 Mar 1;76(3):249-258. doi: 10.1001/jamapsychiatry.2018.4288. PMID: 30698636; PMCID: PMC6439818.
Neurodegenerative Diseases — Concussion Alliance
Gabbe, B., Ayton, D., Pritchard, E. K., Tsindos, T., O'Brien, P., King, M., Braaf, S., Berecki-Gisolf, J., & Hayman, J. (2018). The Prevalence of Acquired Brain Injury Among Victims and Perpetrators of Family Violence. Brain Injury Australia. https://www.braininjuryaustralia.org.au/wp-content/uploads/BRAININJURYAUSTRALIAfamilyviolencebraininjuryFINAL.pdf
_edited.jpg)



Comments